
Everything you need to know about having an endoscopy
From what happens during an endoscopy to how long it takes to recover, we answer key questions about this procedure.
What is an endoscopy?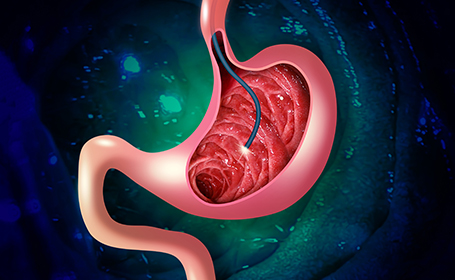
An endoscopy is a procedure that allows a Consultant to see inside the body. The endoscope itself is a thin, flexible tube with a camera and a light source on the end (as well as a surgical instrument, if you’re having an operation).
What does an endoscopy show?
This procedure can be used to investigate unusual symptoms or treat a range of conditions. It can also be performed to carry out a biopsy, where a small tissue sample is taken for further analysis.
Why might you need an endoscopy?
An endoscopy might be suggested if you’re experiencing any of the following symptoms:
- Difficulty swallowing
- Abdominal pain
- Persistent nausea, vomiting or diarrhoea
- Unexplained weight loss
- Vomiting blood
- Blood in stools
- Chest pain that’s unrelated to heart conditions
A modified endoscope with tiny surgical instruments attached to them can be used to:
- Remove gallstones, kidney stones and bladder stones
- Remove small tumours and growths – both cancerous and benign
- Repair damaged joints
- Repair bleeding stomach ulcers
- Insert a stent into an area which is blocked or too narrow to function efficiently
- Tie and seal the fallopian tubes as part of female sterilisation.
What are the different types of endoscopies?
There are several different types of endoscopies. The type of endoscopy you have will depend on the symptoms you’re experiencing.
Here are some of the different types:
- Gastroscopy – this is used to examine the oesophagus, stomach or first part of the small intestine
- Colonoscopy – this is used to examine the bowel
- Hysteroscopy – this is used to look at the uterus
- Cystoscopy – this is used to investigate the inside of the bladder
- Bronchoscopy – this is used to examine the airways
- Endoscopic ultrasound – this is used to produce images of internal organs
If you need an endoscopy, your consultant will give you instructions to make sure you’re fully prepared before the procedure takes place.
How to prepare for an endoscopy
If you need an endoscopy, your consultant will give you instructions to make sure you’re fully prepared before the procedure takes place. It’s always important to tell your consultant about any medications you’re taking. You may need to stop taking certain medications, such as blood-thinners. However, it’s important not to stop taking your prescription medication unless your consultant advises you to do so.
What happens during an endoscopy?
Depending on which part of your body needs to be looked at, an endoscope may be inserted through your mouth, back passage, or through a small incision in your skin. You may have a local anaesthetic to numb one part of your body or you might be offered a mild sedative to help you relax.
Is an endoscopy painful?
An endoscopy isn’t painful, but most people experience a little bit of discomfort similar to a sore throat or indigestion.
What happens after an endoscopy?
After an endoscopy, you will need to rest for about an hour to let the effect of any anaesthetic or sedative wear off. Once this has worn off, you should be able to go home. You don’t need to stay overnight for this procedure. If you do decide to take a sedative, you will need to be taken home by a friend or relative – you shouldn’t drive for the rest of the day.
Your doctor will advise you on when you’ll find out the results from your procedure. If necessary, you may be referred to a different specialist for ongoing diagnosis or treatment.
When can you expect your endoscopy results?
Following the test, there will be a period of recovery for those who have had sedation and the opportunity to relax with a well-earned cup of tea and a snack.
In the vast majority of cases we are able to give you a final report on the day, although samples sent to the laboratory to examine under a microscope will typically take a week to come back.
It is a safe, straightforward procedure and most people can be told their results on the day.

A Consultant's view on preparing for an endoscopy and recovery
Consultant Gastroenterologist, Mr Gareth Parkes from The London Independent Hospital, offers his advice on how to prepare for an endoscopy and what to expect after the procedure.
Don’t forget to fast before your colonoscopy
"My first piece of advice would be not to worry – thousands of gastrointestinal (GI) endoscopies are performed in Circle Health Group hospitals each week. It is a safe, straightforward procedure and most people can be told their results on the day. Prior to arrival be careful to read any information in advance, paying particular attention to any dietary advice. For those having a colonoscopy the bowel preparation and fast can be difficult, but doing it right first time is really important to have clear views. Interestingly some patients feel much better after the preparation and think of it as a complete gut detox!"
Wear comfortable clothing and bring your normal medication
"On the day, I would recommend to wear comfortable clothing and carry a list of your usual medications if you struggle to remember them all."
Plan ahead by having your friends or family collect you
"If you are planning on having sedation remember that you won’t be able to drive, operate heavy machinery or sign a legal contract for 24 hours, so plan in advance and ensure a friend or family can pick you up afterwards. Sedation is not the same as a general anaesthetic; it aims to keep you comfortable and relaxed. If you are finding the procedure difficult or are unusually nervous let the endoscopist know and they can adjust the dose.
"Prior to the endoscopy your consultant will explain the procedure and the small risks involved and ask you to sign a consent form. This is your opportunity to ask questions and deal with any concerns. Just ask your doctor or the nursing team as they are always happy to help."
Your endoscopy with Circle Health Group
Several of our hospitals contain specialist endoscopy suites offering a range endoscopy services.
If you would like to book your endoscopy with Circle Health Group, please contact a member of our team by calling us or booking online.
Tags
How do I book an appointment?
If you're concerned about symptoms you're experiencing or require further information on this subject, talk to a GP or see an expert consultant at your local Circle Hospital.