
About cataract surgery
Cataracts occurs when cloudy patches form on the lens of your eye. We explore the symptoms of cataracts and available treatment options from a new pair of glasses to cataract surgery. We also look at ptosis (the drooping of your upper eyelid) and possible treatments.
What is a cataract and how is it formed?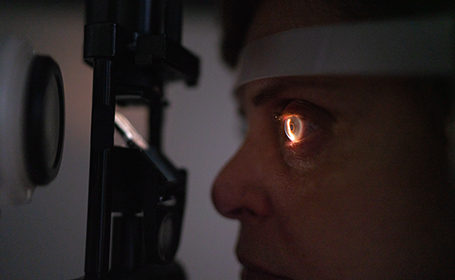
The eye works just like a camera and has a lens that helps us focus the light on to the retina. This lens is located behind the iris, the coloured part of the eye. Clouding of this lens is called a cataract. This haziness of the lens reduces the quality of the image formed on the retina. In over 90% of patients, cataract formation is due to the ageing process. Injury to the eye, certain diseases and some types of medication can also cause cataract formation.
What are the symptoms of a cataract?
A cataract prevents the formation of a sharp image on the retina along with reducing the amount of light going into the eye. This can cause difficulty in reading in dim light, cloudy or blurry vision and fading of colours. Some patients may notice glare from oncoming headlights. A frequent change in the prescription of your glasses is also one of the signs of cataract formation.
Symptoms of early cataract may be corrected with a new pair of glasses, brighter lights or magnifying glasses. If these measures do not help then cataract surgery is the only option.
How is a cataract detected?
A cataract is detected by a thorough eye examination that will include testing your vision with and without your glasses. Special drops are then instilled into the eye to enlarge the pupil. Following this a slit-lamp (special eye examination device) is used to examine all parts of the eye. The dilating drops cause blurring of vision that can last several hours so make sure to have someone to drive you to the consultation. If you are over the age of 60, a detailed eye examination is recommended every 2 years.
What are the treatment options?
Symptoms of early cataract may be corrected with a new pair of glasses, brighter lights or magnifying glasses. If these measures do not help then cataract surgery is the only option. This involves removing the cloudy natural lens and replacing it with an artificial lens. This needs to be done only once, as a cataract is not something that grows back. When you note that the reduction in vision, glare, etc. are starting to interfere with everyday activities like driving and reading, it is time to think about cataract surgery.
Are there any alternatives to surgery?
Your consultant ophthalmic surgeon will explain all the benefits and risks and help you make your decision about proceeding with surgery. There are no drops, vitamins or supplements that can make the cataract go away once it has formed.
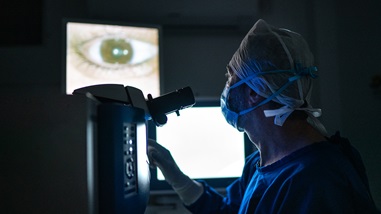
How is cataract surgery performed?
For most patients, cataract surgery is done under local anaesthesia. A tiny incision is made in the eye and through this incision the surgeon inserts an ultrasonic instrument, about the size of a pen tip. This gently breaks up and removes the cloudy lens. Once the clouded lens has been removed, an intraocular lens (or IOL) is inserted permanently to restore the focusing strength of the eye. Cataract surgery is an outpatient procedure.
You'll spend just a few hours at the hospital. Because your eyes will be treated with anaesthetic, you should feel little to no discomfort. After the surgery, you'll be able to go home the very same day. Drops will be prescribed to guard against infection and help your eyes heal. For a few days, you may need to wear a clear shield, especially at night, to prevent you from rubbing your eye.
What causes ptosis? (droopy eyelid)
Ptosis (pronounced TOE-sis) is the term for drooping of the upper eyelid. A person with ptosis may not be able to lift one or both upper eyelids completely. In adults over the age of 40 years, the most common cause is the stretching or loosening of the tendon that lifts the upper eyelid. Ptosis can also occur following routine cataract surgery. It can occur in younger people who use contact lenses.
Neurologic, neuromuscular, or mechanical causes as well as injuries may cause a droopy eyelid. Ptosis may affect one or both eyes and can be very asymmetrical depending on the underlying cause. Difficulty in reading and driving are common complaints. Patients may also notice a loss of the upper field of vision. Raising the entire brow with the muscles of the forehead and scalp may cause headaches and eyestrain.
What treatment is available?
The most common treatment is ptosis surgery, and there are a number of possible approaches. The goal is to tighten the tendon so that the lid is elevated to match the lid on the other side, but with a minimum of scars and side effects. Neurologic and neuromuscular cases may improve spontaneously or respond to treatment of the underlying cause. In adults the surgery is done under local anaesthesia. An incision is made in the upper lid skin crease (almost completely invisible after a few weeks). The levator muscle is identified and re-attached to the lid and the incision closed with very fine sutures.
Most people feel ready to go out in public (and back to work) in about 10 days.
What does the recovery involve?
A wound dressing, if applied, remains in place overnight. Applying an ice pack for the first 48 hours helps reduce post-operative swelling. You will be prescribed with an antibiotic ointment and lubricating eye drops for the first week. You should be able to read or watch television after one or two days. You will usually be reviewed 7-10 days post-operatively to make sure the wound is healthy and to remove stitches. A final visit is carried out eight to ten weeks after surgery.
Most people feel ready to go out in public (and back to work) in about 10 days.
When should I consider cataract surgery?
Although most people with cataracts will need to have surgery at some point, there is no need to have an unnecessary operation to remove a cataract that doesn't affect your life. A cataract should not be removed just because it is there. It doesn't become any more difficult to remove a cataract if you decide to wait before having the operation.
However, there is also no need to delay surgery. A cataract can be removed at any stage of its development; you don't need to stick it out until the last possible moment if you don't want to. The decision to have cataract surgery will depend on a number of factors, including the effect on your eyesight, and the knock-on impact on the rest of your life.
Here are some signs that it might be the right time to get cataract surgery:
- If your vision is making it difficult to read road signs while you're driving
- If you have another eye condition which can't be monitored or treated properly if you have cataracts
- If you're finding it hard to keep up hobbies which require good eyesight, such as reading, knitting or playing card games
- If the cataract is very advanced it can be firmer and harder to remove – in this situation it is safer to remove the cataract sooner rather than later
- If a cataract is causing inflammation or pressure within the eye, it can lead to glaucoma and permanent loss of vision. However, this is a rare scenario and only occurs with very advanced cataracts.
If you don't need or want surgery immediately, there are other steps you can take to improve your vision in the short term (although surgery is the only way to get your vision back fully). You might want to try:
- New glasses or anti-glare sunglasses
- Brighter lighting in your home
When is cataract surgery recommended
It used to be encouraged for people with cataracts to wait until they could hardly see before getting surgery. However, you can now get surgery if your vision is affecting your daily life in any way. If you have cataracts in both eyes, you will have two operations a few weeks apart.
However, there are some circumstances in which a surgeon might want to delay surgery, including:
- If they have concerns about the health of your eyes due to another health condition
- If the risks of surgery outweigh the benefits. All surgery carries risk, and if you only have sight in one eye your surgeon may want to delay until your vision worsens, to make sure the benefits of surgery outweigh the risks.
It's your decision
Ultimately, whether you want to have surgery at the first sign of blurry vision or delay the operation as long as possible, it's your right to do so. The decision of when to have cataract surgery is down to the patient, and although a surgeon can advise you they should never put pressure on you either way.
Tags
How do I book an appointment?
If you're concerned about symptoms you're experiencing or require further information on this subject, talk to a GP or see an expert consultant at your local Circle Hospital.